Everything You Need to Know About Ketamine Infusion Therapy
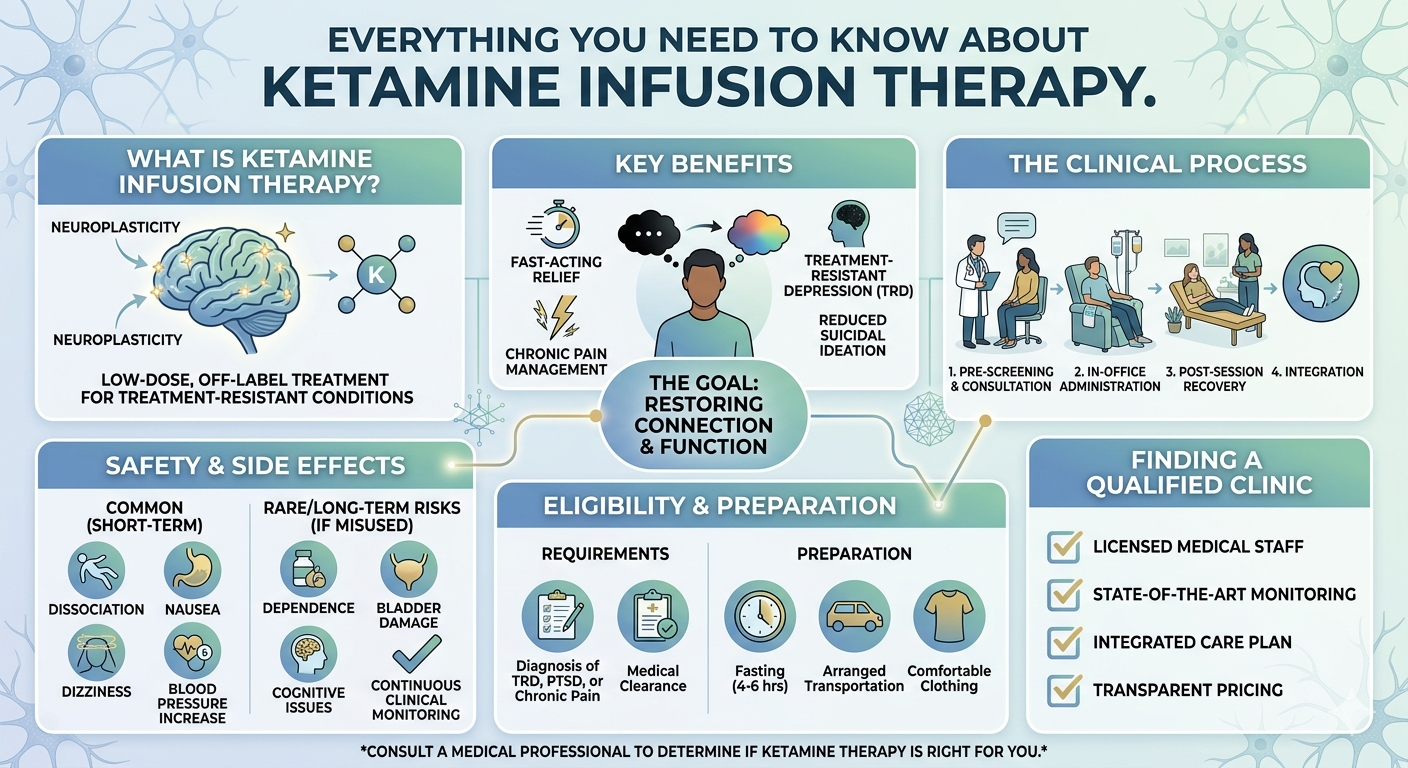
Ketamine Infusion Therapy has become one of the most talked-about treatment options for people living with depression, especially when standard antidepressants have not worked well enough. Depression can affect mood, sleep, focus, appetite, relationships, and the ability to function day to day. For many patients, therapy and oral antidepressants help. For others, the results are slow, incomplete, or frustratingly inconsistent. That is where ketamine infusion has entered the conversation.
Depression is a major global health issue. The World Health Organization reports that about 5.7% of adults worldwide live with depression, and it can interfere with work, relationships, and basic daily life. In the United States, the National Institute of Mental Health reported that 21 million adults had at least one major depressive episode in 2021, representing 8.3% of U.S. adults. These numbers show why new treatment options matter, especially for people who feel stuck after trying the usual path.
What Ketamine Infusion Therapy Actually Is
Ketamine was first used as an anesthetic, but researchers later found that lower, carefully controlled doses may have fast-acting antidepressant effects in some patients. In mental health care, ketamine infusion usually refers to intravenous ketamine administered in a clinical setting under professional supervision.
This is not the same as taking a daily antidepressant at home. During treatment, ketamine is delivered through an IV over a set period, often while the patient sits or reclines in a calm treatment room. A trained clinical team monitors vital signs, comfort level, and response during the session. After the infusion, patients are observed before leaving.
The main reason Ketamine Infusion Therapy gets attention is how differently it works compared with many traditional antidepressants. Most standard medications focus on serotonin, norepinephrine, or dopamine. Ketamine affects the glutamate system, which plays a major role in brain signaling, mood regulation, and neuroplasticity. In simpler terms, it may help the brain form new patterns of communication when depression has kept it locked in the same negative loop.
Research reviews have found that a single subanesthetic IV ketamine infusion may improve depressive symptoms rapidly, sometimes within one day, in some people with major depressive disorder. Other clinical reviews have also reported rapid antidepressant effects in treatment-resistant depression after IV ketamine, though effects may vary and may not last permanently after one session.
Who May Be a Candidate for Ketamine Infusion?
Ketamine infusion is usually discussed for people with difficult-to-treat or treatment-resistant depression. This often means a patient has tried multiple standard treatments, such as oral antidepressants or therapy, without enough improvement. It may also be considered in certain clinical settings where faster symptom relief is important, but the decision should always come from a qualified provider.
A proper evaluation matters. A therapist or prescribing provider may review medical history, psychiatric history, current medications, blood pressure, substance use history, and safety risks before recommending treatment. Ketamine is not suitable for everyone. People with certain cardiovascular conditions, uncontrolled blood pressure, psychosis history, or active substance misuse concerns may need a different approach.
This is where the hype around ketamine needs a reality check. It is not a wellness shortcut. It is not a magic reset button. It is a serious treatment that should be handled with the same level of caution as any other medical intervention. The strongest results usually come when ketamine is part of a broader care plan that may include therapy, medication management, lifestyle changes, and long-term monitoring.
A real-life example makes the need clear. Someone may try one antidepressant, wait six weeks, feel little change, switch to another, deal with side effects, try therapy, improve slightly, then crash again. After months or years of this cycle, the issue is not laziness or lack of effort. Sometimes the treatment model simply has not matched the biology of the condition. Ketamine gives some patients another clinical pathway to explore.
What Happens During the Treatment Process?
The treatment process usually starts with a consultation. The provider evaluates symptoms, previous treatments, health risks, and goals. If the patient appears eligible, the clinic explains the protocol, possible side effects, session length, and aftercare instructions.
During the infusion, ketamine is delivered through an IV at a controlled dose. The patient may feel relaxed, detached, dreamy, or emotionally distant from normal thoughts. Some people describe the experience as calming. Others find it strange or intense. Clinical monitoring is important because ketamine can temporarily affect perception, blood pressure, coordination, and alertness.
Common side effects may include nausea, dizziness, dissociation, increased blood pressure, blurred perception, or fatigue after the session. These effects are usually temporary, but they are the reason patients should not drive themselves home afterward. Most clinics require someone else to provide transportation.
The number of sessions varies. Some protocols use a series of infusions over several weeks, followed by maintenance sessions if the patient responds well. Progress should be tracked carefully using symptom scales, patient feedback, and clinical judgment. Good clinics do not just ask, “Do you feel better?” They measure function, mood, sleep, energy, safety, and relapse patterns.
Why Ketamine Infusion Therapy Matters
The importance of Ketamine Infusion Therapy comes from the population it may help: people who have not responded well to traditional care. Treatment-resistant depression is a serious clinical challenge. Research has estimated that at least 30% of people with depression may experience treatment-resistant depression, which means standard treatment attempts do not produce enough relief.
That number is huge. It means millions of people are not being dramatic when they say the usual options have not worked. They are describing a known treatment gap.
Ketamine infusion also matters because it has pushed mental health care toward faster-acting and mechanism-based treatment. Instead of assuming every patient should follow the same medication ladder forever, providers are now looking more closely at brain pathways, treatment response patterns, and individualized care.
Still, the treatment has limits. Some patients respond strongly, some partially, and some not at all. Benefits may fade without follow-up care. Cost can be a barrier. Insurance coverage may vary. Access depends on location and provider availability. Patients should ask clear questions before starting: Who administers the infusion? What dose model is used? How are side effects handled? How is progress measured? What happens after the first treatment series?
Conclusion
Ketamine Infusion Therapy has earned attention because it offers a different option for people with depression who have not found enough relief through standard treatment. It works through a different brain system, may act faster for some patients, and is administered under clinical supervision rather than taken casually at home.
The key is responsible use. Ketamine infusion should be guided by qualified professionals, supported by careful screening and connected to a broader mental health plan. It is not a cure-all, but for the right patient, it may open a door that traditional treatment could not.
Anyone considering Ketamine Infusion Therapy should speak with a licensed therapist, psychiatrist, or qualified provider to understand the benefits, risks, cost, and eligibility. Depression care should be serious, personal, and honest. When the standard path is not enough, exploring evidence-based alternatives can be a smart next step.





