Is Pityriasis Rubra Pilaris Genetic?
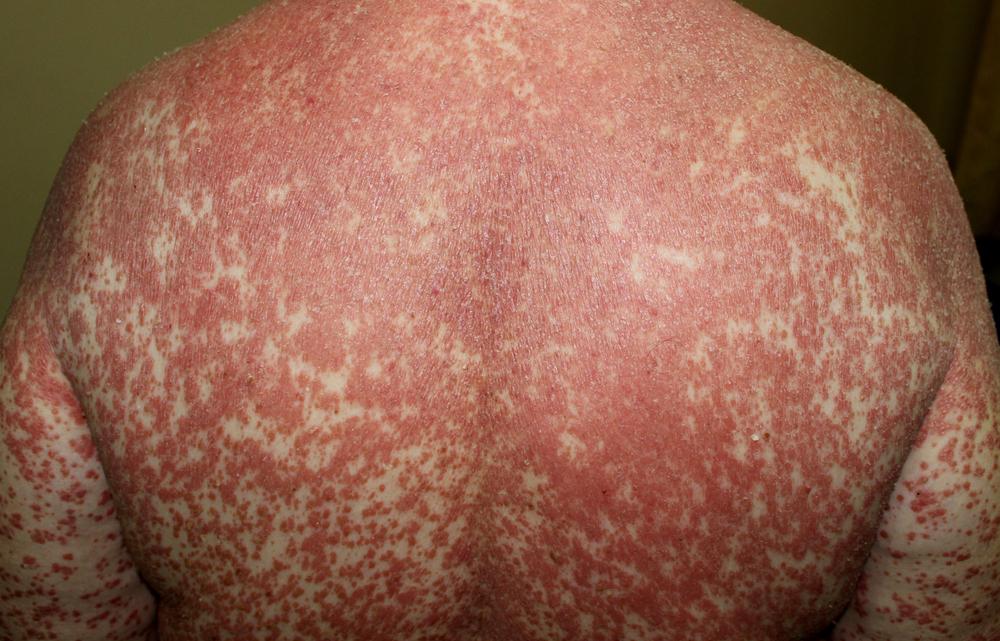
If you’ve noticed reddish-orange patches, thickened palms or soles, or rough bumps on your skin, you may be wondering whether these symptoms point to something more serious, like pityriasis rubra pilaris (PRP). It’s natural to question whether this rare skin condition is inherited or caused by other factors. In this blog, we’ll explore what PRP is, the role genetics may play, potential triggers, how it’s diagnosed, and available treatments. We’ll also touch on ongoing research that could help expand options for people living with PRP.
Understanding whether PRP is genetic can guide how you manage it and what to expect. We’ll also discuss the treatment option for pityriasis rubra pilaris that doctors typically consider for managing symptoms.
What Happens in PRP?
PRP is a rare skin disorder that can significantly affect daily life. It typically presents as reddish-orange patches that may gradually spread across the body. The skin can become thickened, especially on the palms and soles, and small bumps often appear around hair follicles.
These changes are more than cosmetic—they can cause itching, discomfort, and sometimes pain when walking or using your hands. PRP affects the skin’s natural barrier, making it more prone to dryness and irritation.
The condition is chronic in many cases, meaning it can persist for months or even years. While the exact cause remains unclear in most instances, understanding PRP’s underlying mechanisms helps explain why researchers are investigating possible genetic links.
Is PRP Passed Down Through Families?
One of the most common questions people have is whether PRP is inherited. The answer is nuanced. There is a rare familial form of PRP that can run in families. In these cases, the condition often follows an autosomal dominant inheritance pattern, meaning a single copy of the altered gene from one parent can cause the disorder.
Researchers have identified certain gene mutations associated with familial PRP, but these cases are uncommon. Most PRP cases are sporadic, appearing randomly without any family history.
Even in familial cases, symptoms and severity can vary significantly between relatives. Some might experience only mild scaling, while others have more widespread involvement. Understanding whether PRP is genetic helps dermatologists provide proper counseling and anticipate potential patterns in family members.
Could Something Else Be Causing Your PRP?
Not all cases of PRP are inherited. Several non-genetic factors may contribute to its development, including:
- Infections – Some viral or bacterial infections have been linked to flare-ups in skin conditions, though evidence for PRP is limited.
- Immune system abnormalities – PRP may involve irregularities in how the immune system regulates skin cell turnover.
- Environmental factors – Certain triggers, like stress, climate changes, or skin trauma, can worsen symptoms.
- Medications – Rarely, certain drugs may provoke or exacerbate PRP-like rashes.
Because triggers vary from person to person, identifying them requires careful evaluation by a dermatologist. Understanding both genetic and environmental factors provides a more complete picture of why PRP develops and how best to manage it.
How Do You Know if It’s PRP?
PRP can be challenging to diagnose because its symptoms resemble other skin conditions, like psoriasis or eczema. Key signs to watch for include:
- Reddish-orange patches that may begin on the scalp or torso and spread outward
- Scaling or thickening of the skin, particularly on palms and soles
- Follicular bumps, often around hair follicles, giving the skin a rough texture
- Itching or discomfort, especially in affected areas
To confirm a diagnosis, doctors usually perform a physical examination and may take a skin biopsy to examine tissue under a microscope. Blood tests are sometimes used to rule out other conditions or detect underlying immune issues. Early diagnosis is important because timely management can prevent worsening and improve quality of life.
What Are the Options for Managing PRP?
Treating PRP requires a tailored approach based on severity, type, and individual response. Doctors consider several treatment options for pityriasis rubra pilaris, including:
- Topical therapies – Emollients, moisturizers, and mild corticosteroids help reduce inflammation, dryness, and scaling.
- Systemic medications – Oral retinoids or immunosuppressants are often prescribed for moderate to severe cases, especially when large areas of skin are involved.
- Phototherapy – Controlled exposure to ultraviolet light can help some patients, although this is not suitable for everyone.
Treatment goals focus on managing symptoms, slowing disease progression, and improving comfort. PRP can be stubborn, and what works for one person may not work for another, so ongoing follow-up with a dermatologist is essential.
Lifestyle habits also play a role. Gentle skin care, avoiding harsh soaps or irritants, and maintaining consistent hydration can support medical treatments and reduce flare-ups. Combining professional care with self-care strategies often leads to the best outcomes.
What’s Next in PRP Understanding and Care?
Research into PRP is ongoing, particularly for the familial form linked to genetic mutations. Understanding these pathways could eventually lead to targeted therapies that address the root cause rather than just symptoms.
Even in sporadic cases, clinical studies are helping researchers identify factors that influence PRP development and treatment response. Participating in research can offer patients access to novel therapies and contribute to a broader understanding of this rare condition.
For those affected, staying informed about new studies and treatment options is empowering. Awareness allows patients and families to make proactive choices and explore potential advancements in care.
Conclusion
PRP can be genetic in rare familial cases, but most instances appear sporadically. Early diagnosis, a personalized treatment plan, and consistent follow-up are key to managing symptoms effectively. By understanding the factors that influence PRP, from genetics to environmental triggers, patients can make informed decisions about care and daily routines.
If you or a loved one is living with PRP, there are opportunities to contribute to research and support the development of better treatments. You can enroll now in palmoplantar keratoderma studies, which help researchers learn more about rare skin disorders, improve therapies, and potentially provide access to advanced care options. Taking part in research is not only empowering but also helps advance understanding for future patients.
With careful management, professional guidance, and awareness of ongoing studies, living with PRP can become more manageable, and patients can maintain a good quality of life despite the challenges of this rare skin condition.



